The importance of timely intervention
It is important to start Duchenne muscular dystrophy (DMD) treatment as soon as possible following a diagnosis, to ensure the best outcomes for patients.1
DMD is caused by a mutation in the gene that codes for dystrophin — a protein that helps to keep muscles working properly.1
As a result, the body cannot make dystrophin and muscles weaken. Over time, this muscle weakness will lead to many health problems. Eventually, the muscles that control the heart and lungs stop working properly.2
The good news is that management and treatment options are available and can have a positive impact on the way DMD progresses. This includes medications, as well as other interventions such as physiotherapy that help maintain muscles and joints.2
Medications can help slow down loss of muscle function and weakness, which may help to delay any complications. This means that your child may stay mobile longer and live more independently than they would without specialised care and management.1,3,4
Early and appropriate DMD treatment can help your child in a number of ways. It may:1–4
- Stop the disease progressing so rapidly
- Help control symptoms
- Help your child maintain their independence and quality of life for as long as possible
How is DMD treated?
Treatments for DMD can be divided into two main groups:1,2

Medications
Medications help slow the loss of muscle function and treat the symptoms of DMD

Supportive care
Supportive care manages the complications of DMD and helps improve a person’s quality of life. This includes things like physiotherapy, heart monitoring and breathing support
Types of medication for DMD

Drugs that help reduce inflammation in muscle cells1,3,5,6
These are the most commonly used medications for DMD. They are used to help maintain muscle strength for as long as possible. They may also keep the heart and lungs strong for longer, as well as delaying the development of scoliosis.
Glucocorticoids are the main type of medication in this category. Treatment with them is usually recommended by the doctor as soon as possible after a diagnosis of DMD, to try to slow down the progress of the disease. However, this type of medication can also cause a number of side effects, including bone damage, weight gain and delayed puberty. Your child’s doctor should be able to provide you with more information on the use of glucocorticoids.

Drugs that help muscle cells produce dystrophin3
DMD is caused by a mutation in the gene that codes for dystrophin — a protein that helps to keep muscles working properly. As a result, the body cannot make dystrophin as normal.
Medications that target the underlying cause of the disease allow the body to make a working form of the dystrophin protein.
The medicines that are currently available in this category are only suitable for some patients with DMD, due to the way in which they work. Therefore, an understanding of the specific mutation causing DMD in a patient may help to determine the right management pathway. This is done through genetic testing and should be completed as early as possible.
Potential new treatment strategies are emerging, some of which are in clinical trials. You should talk to your child’s doctor about treatment options because they are best placed to advise you on medical matters.

Heart medications5
People with DMD may develop a heart problem called cardiomyopathy, which reduces the heart’s ability to pump blood around the body. Eventually, heart failure may develop.
The main treatments for heart disease are medications known as angiotensin converting enzyme (ACE) inhibitors and angiotensin receptor blockers (ARB). These medications are generally started as soon as a patient shows evidence of heart failure, either through symptoms or following tests that scan the heart and can spot if something is wrong. An echocardiogram and a cardiovascular MRI (magnetic resonance image) are the two most commonly used heart imaging scans used in children with DMD. If you have concerns about heart problems with your child, ask the doctor for more information on cardiomyopathy and how it is managed.

Bone medications5
People with DMD often have weak bones and may develop a condition called osteoporosis. This makes the bones fragile and more likely to break.
Osteoporosis can develop for a number of reasons. Muscle weakness and the use of certain medications contribute to bone weakness.
Bone strength can be increased through the use of medications called bisphosphonates. These are typically given as an injection at the first sign of any bone fragility, such as fractures or bone damage spotted on X-rays. Early treatment is important in order to preserve normal bone development, particularly the spine. If you have any concerns, your doctor should be able to provide you with more information on bone health in DMD.

Vaccinations3,5
Because people with DMD often have trouble coughing, chest infections are more common. This is because coughing helps clear mucus and germs from the respiratory tract.
Influenza (flu) and pneumococcal (pneumonia) vaccines may be offered. These vaccinations help prevent chest infections from happening in the first place.
Types of supportive care for DMD
Managing DMD takes more than just medication. Because DMD weakens muscles throughout the entire body, it has a variety of effects on different body systems. This makes people with the disorder more susceptible to complications.1
The best way to manage DMD involves a combination of approaches and a team of different specialist doctors, nurses and healthcare professionals.1

Muscle health1,7,8
Because DMD causes the muscles in the body to become weak and damaged, maintaining muscle strength and function is a key part of care.
Physiotherapists, occupational therapists and other rehabilitation specialists play a major role in the care of people with DMD. They work on stretching out the muscles and keeping joints as flexible as possible.
Braces may be used to provide additional support for joints, typically the ankle, foot or knee. Sometimes a special type of brace may be recommended for your child while they sleep, which keeps their feet pointing downwards to help stop the Achilles tendon from becoming tight.
Standing is generally recommended for a few hours each day. This is because it can help promote better circulation and healthier bones, and also help maintain a straight spine. For children who need assistance, a standing walker or frame may be recommended.
As DMD progresses, a scooter, stroller or wheelchair may be needed to help your child get around and be more independent. Although many parents have understandable concerns if their child needs to start relying on a wheelchair to get around, many find that their child actually becomes much more mobile and energetic than they were before.
Many other types of mobility aid are available that can help as your child requires more and more assistance. These include wheelchair transfer boards, shower chairs and electronic beds. Talk to your child’s doctor or physiotherapist for more information on what help is available to you.
Specific surgical procedures may also be recommended for muscular symptoms that greatly interfere with a patient’s day-to-day life. If the muscles around the eye become weak, surgery can be used to lift droopy eyelids and improve a patient’s vision. Tendon contracture, when the tendons in a joint become short and tight, may be surgically loosened to increase their flexibility. Mobility in weak shoulder muscles may be improved by a surgical procedure known as ‘scapular fixation’, which involves attaching the shoulder blades to the back of the ribs.
Exercise1,6,7
Regular exercise is important in children with DMD to keep their muscles as strong as possible. However, exercises that put too much stress on the legs (e.g. trampolining or activities that involve squatting, etc.) should be avoided as these can lead to muscle injury. Moderate, low-impact exercise for a short amount of time, so that your child doesn’t become too exhausted, is usually recommended.
Swimming and other swimming-pool-based activities are generally considered an ideal exercise choice for children with DMD, as the water helps reduce the amount of strain placed on the muscles. However, it’s always best to talk with the child’s doctor and physiotherapist to work out the most suitable exercise plan for your child.
Diet1
DMD affects all muscles in the body, including the muscles that help control eating, swallowing and digestion. This can cause constipation and gastroesophageal reflux, as well as make chewing and swallowing difficult (sometimes referred to as ‘dysphagia’). If these are persistent and do not get better following changes to your child’s diet, medications may be prescribed to help keep them under control.
A healthy diet and weight are especially important for children with DMD. A dietitian will help make sure that your child receives a well-balanced diet and the right amount of nutrients, supplements and fluids. A gastroenterologist will also be able to help with any digestive problems.
As being obese or underweight/malnourished can occur as a result of both DMD itself and the medications used to manage it, your child should receive regular growth and weight assessments to ensure they are healthy. You can always talk to your child’s doctor or dietician if you have any concerns about your child’s weight.

Bone health5
Children with DMD often develop a condition called osteoporosis. This makes the bones fragile and more likely to break. As back muscles become weaker, the spine may also begin to curve — this is known as scoliosis.
Children with broken bones (fractures) in their spine can often show no symptoms, even when the fracture is severe. Scans such as X-rays are therefore used to detect the earliest signs of bone damage. Early detection of fractures is important to prevent further injury and also to identify children who are prone to fractures, as they may require more regular monitoring for bone damage.
The presence of scoliosis will usually be assessed at least once a year by your child’s doctor. It is generally assessed by simply looking at the child’s back to see if it curves to the side and, if suspected, the diagnosis is confirmed using an X-ray.
Medication may be used to treat osteoporosis. Surgery or casting may also be offered in the case of fractures or scoliosis.
Breathing support5
The muscles used for breathing are also affected by DMD. As the disease progresses, these muscles get weaker and people with DMD start to have trouble breathing and coughing.
Your child will receive regular tests to ensure that their lungs are working correctly and that they are not experiencing any breathing problems. Breathing problems can be reduced by various machines that help the lungs to breathe (ventilators) and cough (cough assist machines). In some cases, ventilation is only required when a child is sleeping, particularly when breathing problems interfere with their ability to sleep.

Heart health5
DMD affects all of the body’s muscles — including the heart. Often the signs and symptoms of heart damage are easy to miss, particularly in children who are no longer able to walk. That is why your child‘s heart health will be checked often by a cardiologist.
The cardiologist may suggest using medication if the heart is damaged — a condition called cardiomyopathy — or to help reduce future damage. It is important that any heart damage is diagnosed and treated as early as possible. If the heart becomes very damaged, it can have a big impact on your child’s health and quality of life.
It is believed around half of female DMD carriers also experience some degree of cardiomyopathy. It is therefore recommended that they undergo a complete cardiac assessment in early adulthood, which is then repeated every 3–5 years. This will usually include a procedure that scans the heart to allow the doctor to see if anything is wrong. The most commonly used heart imaging scans are an echocardiogram or a cardiovascular MRI.

Learning2,3,9
Dystrophin proteins have been found in the brain. The role that they play is unclear, but this could help explain why problems with learning, speech and behaviour tend to be more common in people with DMD.
A number of different mental health professionals will be able to provide support, depending on the person’s individual needs. Schools will also be able to adapt to both physical and learning needs.
Which healthcare professionals are involved in DMD care?
Receiving a diagnosis of DMD can be difficult, but you are not alone. Your care team is there for you and will be able to offer information and support as you need it, so please reach out to them.
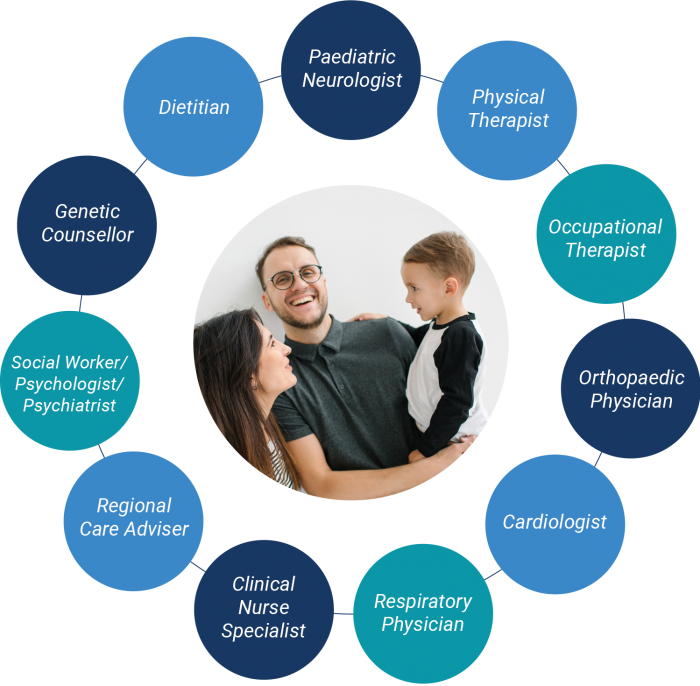
Your DMD care team may include the following:1,5,10
Neurologist / Neuromuscular specialist
A doctor who specialises in conditions that affect the brain, spinal cord and nerves. This doctor often directs and coordinates the DMD care team.
Physiotherapist
A health professional who works with patients to improve muscle and joint function.
Occupational therapist
A health professional who helps children develop the skills to perform everyday activities.
Orthopaedic physician
A doctor who specialises in bone and joint disorders.
Cardiologist
A doctor who specialises in diseases of the heart.
Respiratory physician
A doctor who specialises in diseases of the lungs.
Clinical nurse specialist
A nurse who specialises in providing care for patients with DMD.
Regional care advisor
A professional who provides social, psychological, emotional and practical support for patients and families with DMD. They also provide guidance on services, equipment and funding.
Social worker / Care worker
A professional who helps families adjust to a DMD diagnosis, putting them in touch with services they might need and working with schools to make sure they have the right equipment and systems in place.
Genetic counsellor / Geneticist
A health professional who specialises in medical genetics and counselling.
Dietitian
A health professional who provides nutritional therapy and/or advice to patients and their families.
Learn more about the benefits of physiotherapy stretches for
Duchenne muscular dystrophy
Physiotherapy stretches for DMD

Physiotherapy stretches for Duchenne muscular dystrophy
As DMD causes muscles to become weak and damaged, maintaining muscle strength and function is a key part of care.

Living with Duchenne muscular dystrophy
Life does not stop with a DMD diagnosis. It is still possible to have a productive, creative and fulfilling life.

Carer support space
Caring for someone with DMD isn’t always easy, however, resources are available to support you.

The ultimate guide to Duchenne muscular dystrophy
Everything you need to know about DMD, all in one place.
References
- Birnkrant DJ, et al. Lancet Neurol. 2018;17:251–267 [Part 1].
- Muscular Dystrophy Association. What is… Duchenne muscular dystrophy. Available at https://www.mda.org/sites/default/files/2020/10/MDA_DMD_Fact_Sheet_Oct_2020.pdf [last accessed October 2022].
- Mah JK. Neuropsychiatr Dis Treat. 2016;12:1795–1807.
- Gloss D, et al. Neurology. 2016;86:465–472.
- Birnkrant DJ, et al. Lancet Neurol. 2018;17:347–361 [Part 2].
- Bushby K, et al. Lancet Neurol. 2010;9:77–93.
- Muscular Dystrophy Association. DMD Medical Management. Available at https://www.mda.org/disease/duchenne-muscular-dystrophy/medical-management [last accessed October 2022].
- NHS Health. Muscular dystrophy – Treatment. Available at https://www.nhs.uk/conditions/muscular-dystrophy/treatment/ [last accessed October 2022].
- Birnkrant DJ, et al. Lancet Neurol. 2018;17:445–455 [Part 3].
- Muscular Dystrophy UK. Neuromuscular team. Available at https://www.musculardystrophyuk.org/get-support/health-and-care/neuromuscular-team [last accessed October 2022].
© 2022 PTC Therapeutics.
GL-DMD-0660 | October 2022